Medical Data Interoperability with HL7 EMR and EHR Standards


Information standardization is the key to effective clinical data sharing between hospitals and different systems in a healthcare organization.
According to statistics, an average medical institution uses 16 diverse software systems. With more than 500 vendors using different technologies, hospitals struggle to exchange clinical data between various systems.
In order to facilitate data interoperability, the HL7 EHR functional model was developed. These days, HL7 standards are widely adopted by many organizations and healthcare software development vendors. In the post below, you will discover what HL7 EHR rules are and what their purpose is.
What Is HL7 For EMR And EHR?
Health Level Seven (HL7) is a set of rules and standards that help standardize clinical data for establishing information interchangeability.
By following the HL7 EHR rules, healthcare organizations standardize all the information and its structure. The approach foresees the opportunity to connect different solutions with EHR systems developed by using various technologies. The HL7 EHR functional model complies with most health data transferring policies, keeping confidential data unexposed.
Example of HL7 message:
“MSH|^~&|KioskApp|KIOSK|HospitalSystem|202409231530||ADT^A04|12345|P|2.3|PID|1||12345^^^KioskSystem||Smith^John||19800515|M|”
While an average person can hardly understand this message, any HL7-enabled system can, enabling the opportunity for software solutions from different vendors to interact and exchange medical data error-free.
The message is from a kiosk to a hospital’s information system aimed at registering a new patient. It describes an event in a unified format and shares the following information:
- Patient’s ID
- Name
- Birth date
- Gender
This type of message triggers the hospital’s information system to create new records with the received information automatically.
HL7 Vision: A world in which everyone can securely access and use the right health data when and where they need it.
HL7, Health Level Seven International
How Is HL7 Used In Healthcare?
The HL7 standards help medical organizations connect systems with different purposes and are built using distinctive technologies.
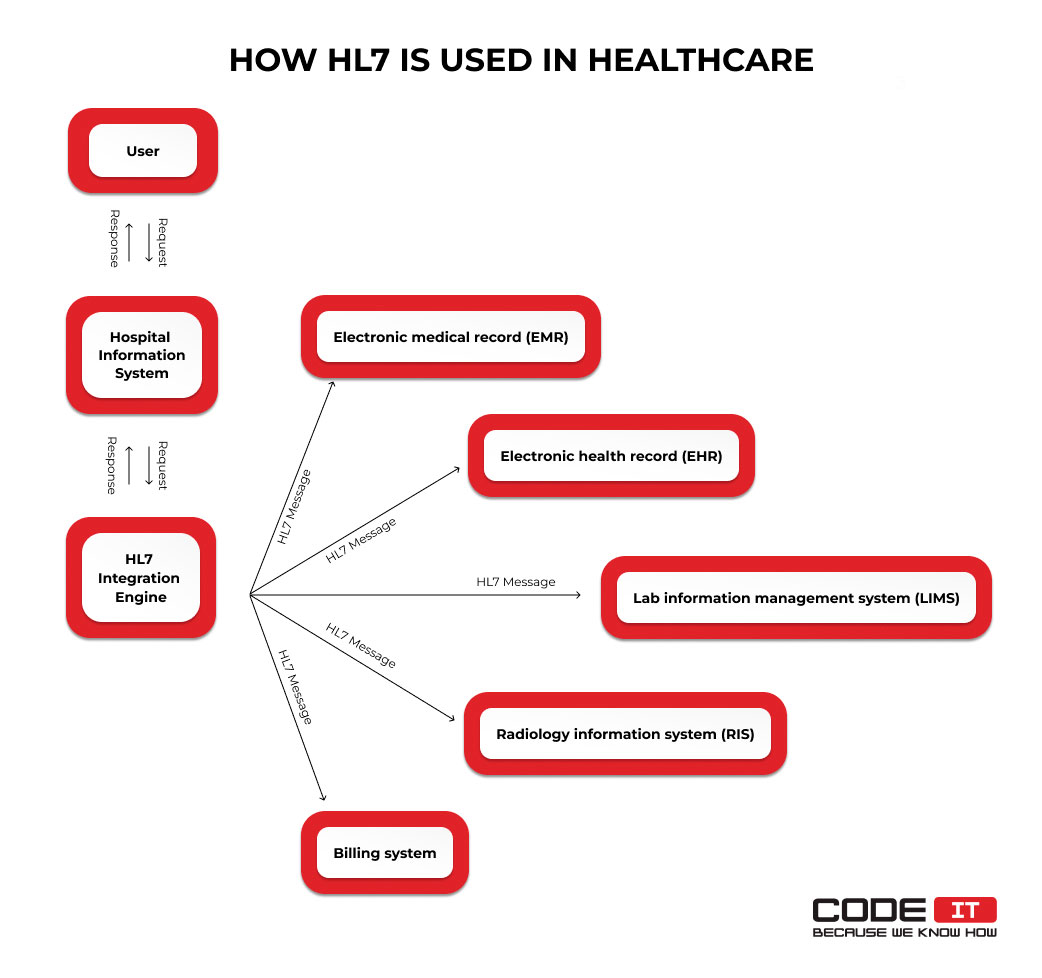
For instance, the rules enable patients, medical staff, and authorized third parties to connect a hospital information app with the following systems:
- Electronic medical record (EMR)
- Electronic health record (EHR)
- Radiology information system (RIS)
- Lab information management system (LIMS)
- Billing system
Let’s check use scenarios to discover how HL7 standards help facilitate health data exchange in real-world environments.
Use Scenario #1: Appointment Check
Let’s check how HL7 standards help patients verify their appointment using a terminal in a medical institution in more detail.
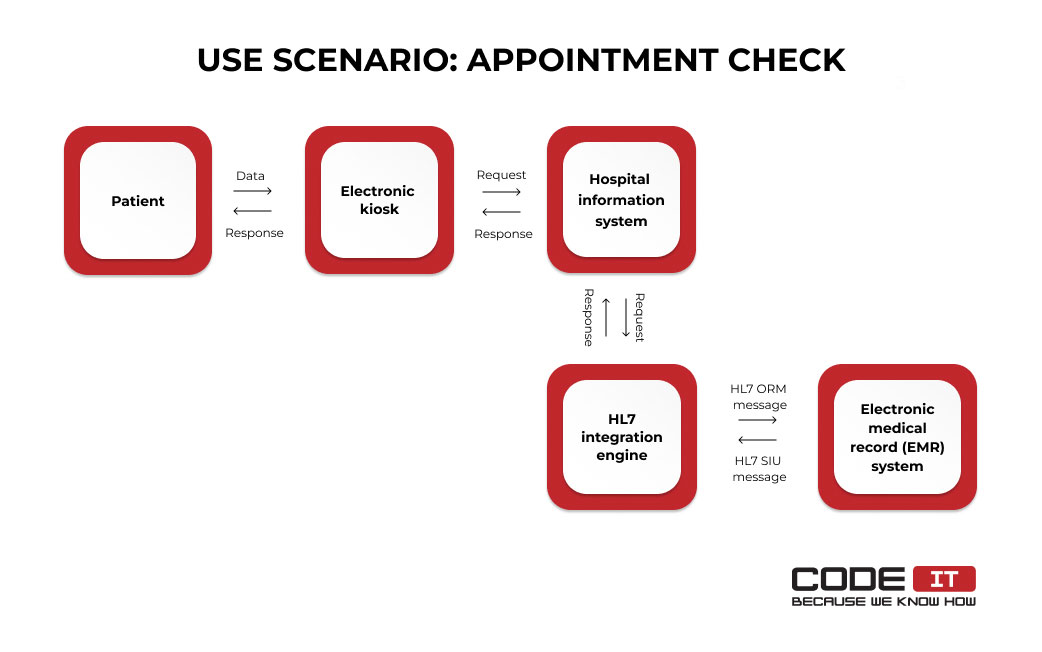
The data flow of the use scenario implies the following actions:
- A patient enters authorization details and requests appointment data using on-site kiosks in a hospital.
- Requests are sent to the hospital information system.
- A web service request is sent to an HL7 data integration engine.
- An HL7 ORM (Order Entry) message is sent to an EMR system.
- An HL7 SIU (Scheduling Information Unsolicited) message is returned.
- A web service response message is sent to the hospital information system.
- Appointment information is delivered to the patient using the kiosk’s interface.
Use Scenario #2: Radiology Results Request
A doctor requests the radiology results of a patient by using a hospital information system.
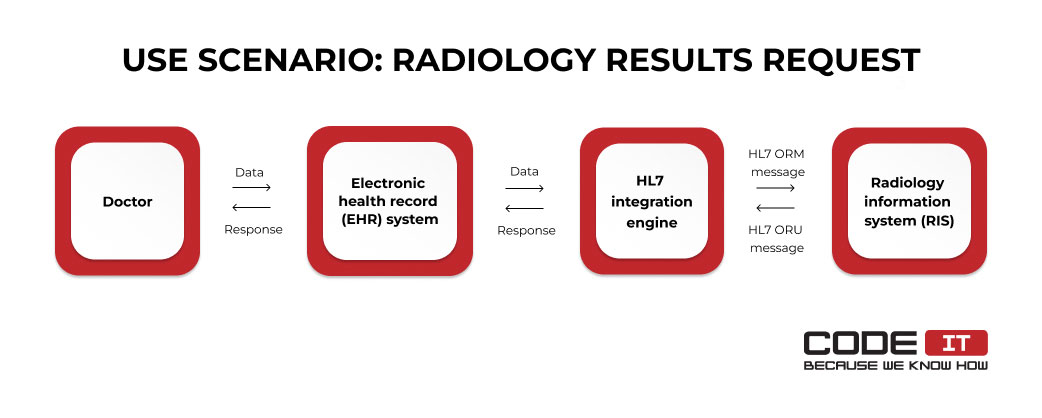
The data flow implies the following stages:
- A doctor uses an EHR system to request radiology results from a RIS.
- A web service request is passed to an HL7 integration engine.
- The request is transformed into an HL7 ORM (Order Entry) message and is sent to a RIS.
- An HL7 ORU (Observation Result) message is sent to the data integration message.
- An EHR system receives a web service response from the engine.
- The radiology results are saved in the EHR system and are analyzed by the doctor.
Use Scenario #3: Prescription Ordering
A doctor submits a prescription order that is sent to a pharmacy dispensing system automatically.
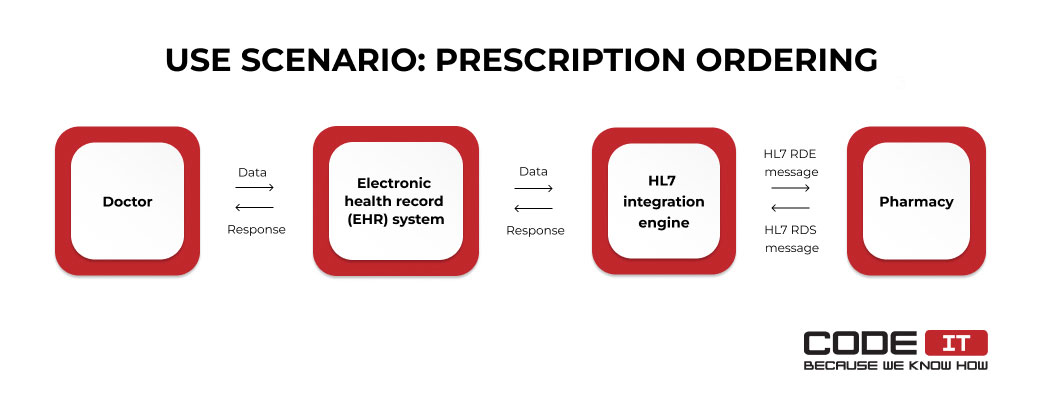
The data flow implies the following stages in this use scenario.
- A doctor submits a prescription order using an EHR system.
- A web service request is sent to an HL7 integration engine.
- The request is transformed into an HL7 RDE (Pharmacy/Treatment Encoded Order) message and is sent to a pharmacy.
- Once the order is fulfilled, a response in the form of an HL7 RDS (Pharmacy/Treatment Dispense) message is returned.
- The response HL7 RDS message is transformed into a web service request and is sent to the EHR system.
Need a custom solution for medical organization?

Business First
Code Next
Let’s talk
How Do HL7 Standards Work?
Let’s elaborate on the HL7 EHR data standards to better understand how they work. The number 7 in the standard’s name refers to the layer it applies to in the OSI model. It includes the following layers:
- Physical — A physical network connection like Ethernet cables, WiFi connection, etc.
- Data link — Data format definition.
- Network — Network management and data routing.
- Transport — Data flow maintenance.
- Session — Ports and sessions control for session management.
- Presentation — Data translation, including encryption/decryption, data compression, etc.
- Application — End-user application with network access.
Developers can use different technologies to implement solutions on layers 1-6. The HL7 data interoperability rules are used on the application layer only.
The HL7 EHR functional model enables healthcare systems to exchange data using messages formatted according to specific clinical data standards. Different software solutions can be connected using an integration engine that turns domain-specific data into HL7 messages.
There are dozens of HL7 message types that help share different kinds of health data. The ten most common types of HL7 V2 messages are the following.
| HL7 Message Type | HL7 Message Name | Description |
|---|---|---|
| ADT | Admit, Discharge, and Transfer | Information about patients in a healthcare facility, events related to patients, personal data updates, etc. |
| ORM | Order Entry | It is a request message type that initiates the transfer of requested details. |
| ORU | Observation Result | A message that implies the observations results of a patient, including lab reports, radiology results, EKG studies, etc. |
| MDM | Medical Document Management | This type of HL7 message enables healthcare organizations to transfer medical documents efficiently, receive change updates, change statutes, etc. |
| DFT | Detailed Financial Transactions | It helps transfer financial information about charges, insurance, billing accounts, charges, and other details to a billing department. |
| BAR | Billing Account Record | This message type helps create new billing accounts, change, and delete them. |
| SIU | Scheduling Information Unsolicited | It is used to share information about patients’ appointments. Also, it can be used to schedule appointments, reschedule or cancel existing ones. |
| RDE | Pharmacy/Treatment Encoded Order | Messages that help doctors submit pharmacy orders and send them to pharmacy dispensing systems fast. |
| RDS | Pharmacy/treatment Dispense | It is a response message from a pharmacy to notify a healthcare organization about a fulfilled order. |
| ACK | Acknowledgment Message | This response message indicates the status of submitted requests or errors that occurred if a recipient didn’t receive a message. |
What is Interoperability in Healthcare, and What are Its Key Benefits?
Versions of HL7 EHR Standards
Many versions of HL7 EMR (electronic medical records) rules use different approaches to health data transferring. HL7 standards define how documents are structured, what data types are used, and what languages are utilized.

The four primary HL7 data standards are the following:
- HL7 Version 2. Many 2.X versions are compatible with each other. HL7 V2 messages are composed by using defined rules and symbols to share clinical data efficiently. It is a legacy standard that lacks some features.
- HL7 Version 3. It is a newer version of the HL7 standards that implies additional features. It uses XML to share messages. Vocabulary data standards, domain-specific modules, and standardized clinical data types are some features of this HL7 standards version. Healthcare providers didn’t widely adopt the version because it is not backward compatible with the 2.X versions.
- CDA. It is the document creation standard that defines rules for composing medical documents. CDA documents have a human-readable format and use defined terminology to achieve semantic interoperability. Documents are structured by using certain standards and are created using templates.
- FHIR. The HL7 Fast Healthcare Interoperability Resources standard is the newest one with many forward-looking features. Structured messages are shared by using APIs. The newest standard enables the opportunity to share clinical data in live time, supports different formats, has a modular structure, and can work with many applications.
Develop Innovative Healthcare Solutions that Use HL7 Standards
Benefits Of Using HL7 In Healthcare
More than 95% of healthcare organizations are about to keep investing in interoperability development or increase their spending due to the many benefits. Let’s check the foremost advantages of interoperability promotion.
Smooth Integration of Different Systems
The usage of HL7 standards enables healthcare organizations to interconnect a lot of systems from different vendors, regardless of the technologies they use.
For example, a hospital can choose a hospital information system (HIS), billing system, and laboratory information management system (LIMS) from different providers and integrate them into one solution for managing patients’ data.
Example: A healthcare provider uses HL7 standards to exchange medical data between an electronic health record (EHR) system, a billing platform, and a laboratory information management system (LIMS). Each system is built by different vendors using diverse technologies. An integration engine helps synchronize data between systems automatically.
Better Data Quality
Thanks to standardization, medical organizations can improve the quality of their data. The adoption of HL7 standards needs hospitals to share messages that match defined standards. Also, they can use templates to create documents for sharing. They can verify and change data shared between different systems using an integration engine through the EMR HL7 interface.
Example: A hospital uses HL7 templates to standardize all the records stored in its database. It helps ensure clinical data is stored in a format that can be easily shared with others. Missing records are highlighted so that the administrative staff can fill them manually.
Improved Collaboration
HL7 standards allow medical organizations to share health data to improve patient care coordination. Clinical data interoperability enables different medical institutions to fetch electronic health records from other hospitals or labs so that patients don’t need to bring lab analysis results or medical records.
Example: A large healthcare network has implemented the HL7 standard to integrate data across its facilities that use diverse digital solutions for managing patient data. The centralized data collection eliminates the need for patients to carry their medical information as it is being simultaneously synchronized across all the facilities of the provider.
Reduced Number of Errors
Since documents or messages are created by following HL7 rules, hospitals can reduce the number of errors caused by human factors.
Besides, the HL7 standards enable medical staff to ensure that messages are delivered. For instance, when using the EMR HL7 interface, systems share the Acknowledgement Message (ACK) to ensure a message is successfully delivered. Otherwise, users receive response messages about failed message delivery and errors.
Example: A hospital has implemented automated data-sharing pipelines, eliminating the need for the administrative staff to input all the records manually. It has helped significantly reduce the number of errors.
Improved Compliance
By implementing HL7-driven digital solutions, hospitals can access a framework that helps securely share digital health information, complying with HIPAA regulations.
The Affordable Care Act (ACA) requires healthcare institutions to exchange health information between different systems electronically. Using HL7 standards, they can seamlessly integrate solutions from different providers into one system to meet all the requirements.
Example: In order to comply with regulations like HIPAA and the Affordable Care Act (ACA), a healthcare provider has implemented HL7 standards so that patient data can be securely shared between systems.
Health Information Exchange Automation
Healthcare organizations widely adopt the HL7 data standards due to the many benefits they offer.
For instance, using HL7 standards, healthcare organizations can develop systems where an electronic health record (EHR) system automatically fetches data from a laboratory information management system (LIMS) when a test is completed.
Example: A hospital uses HL7 standards to automate the exchange of patient data between their EHR and laboratory systems. When lab test results are ready, they get automatically sent to the EHR.
How Electronic Health Records Improve Patient Care
HL7 Interoperability Challenges
The incorporation of HL7 standards need healthcare providers to resolve a lot of issues. They need to map out all the data used by their systems and define where it is recorded. Also, they have to create data-sharing pipelines which may be challenging if they utilize legacy systems built using outdated technologies.
1. Insufficient Standardization
Healthcare providers usually use custom-built software solutions that have distinctive architectures and are built with different technologies. Hence, there is a lack of standardized solutions for integrating HL7 support into a clinic’s workflows. Moreover, some legacy systems that were not built with interoperability in mind may make it difficult for software engineers to understand how it works, where it fetches data, and how it stores new records.
How to overcome:
Hire an experienced HL7 integration vendor with deep expertise in analyzing legacy systems and implementing data transformation tools. Also, you may switch to using other software tools that support the HL7 standard.
2. Incomplete Datasets
The success of interoperability heavily relies on sharing complete and error-free records in defined format. Since many healthcare providers use fragmented or incomplete datasets, where crucial patient information such as medical histories or lab results are missing. Also, hospitals may store data in specific format that can be hardly formatted or lead to missing data when transformed.
How to overcome:
Implement clear data collection and validation workflows. Also, run medical record audits to ensure no data is missing and match the defined requirements.
3. Isolated Systems
Hospitals may utilize isolated solutions for storing different types of data about a single patient and import/export all the records manually. For instance, each department uses a distinctive digital system tailored to specific workflows. The systems are not integrated so that employees need to manually export/import patient information that needs to be shared across different departments.
How to overcome:
Develop and implement integration engines to enable automated data-sharing pipelines. Create cloud-based solutions to make a centralized system for storing and analyzing medical records.
4. Technical Complexity
The integration of HL7 standards requires deep technical expertise. Healthcare providers need to hire certified developers and business analysts with hands-on experience in defining data sources and implementing data transformation tools to automatically compose messages following HL7 guidelines. Moreover, software engineers need to consider the compatibility issues of different versions of the HL7 standard.
How to overcome:
Hire business analysts to thoroughly analyze data sources and create detailed reports to understand how records are organized, considering the architecture of a defined system. Moreover, invest in training and HL7 certification for your internal software development team.
HL7 EMR And EHR Statistics
The HL7 standards are widely adopted by healthcare organizations due to the many benefits they offer.
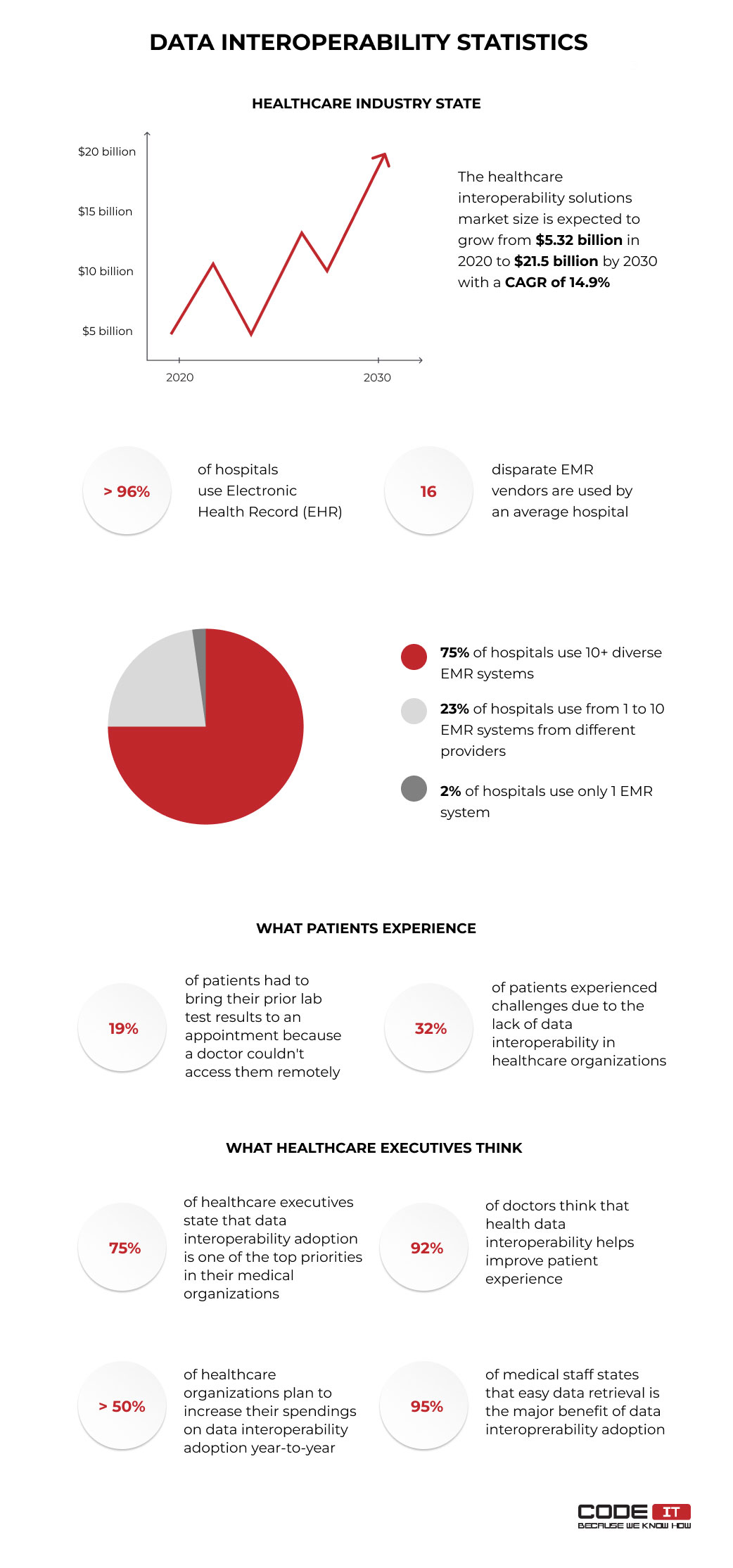
Take a deeper look at the state of health data interoperability by examining overall health data interoperability statistics.
- The data interoperability market size is estimated to reach the $21.5 billion milestone by 2030 at a CAGR of 14.9%, according to Allied Market Research.
Explore the major problem that patients face due to the lack of data interoperability in medical organizations by checking the statistics that are gathered by the National Coordinator for Health Information Technology (ONC).
- 19% of patients had to bring their prior lab test results to an appointment because a doctor couldn’t access them remotely.
- 32% of patients experienced challenges due to the lack of data interoperability in healthcare organizations.
Also, let’s discover what healthcare executives think by checking the statistics below.
- Google states that 75% of healthcare executives state that data interoperability adoption is one of the top priorities in their medical organizations.
- According to the research conducted by the Google Cloud team, 92% of doctors think that health data interoperability helps improve the patient experience.
- Insider Intelligence found that more than 50% of healthcare organizations plan to increase their spendings on data interoperability adoption year-to-year.
Key Takeaways
The HL7 EHR framework sets standards that enable medical organizations to share health data fast and error-free. The main objectives of implementing these data interoperability standards are as follows:
- Integrate HL7 data from EHR system
- Comply with regulatory requirements
- Improve patients experience
There are many versions of HL7 standards. The FHIR is the newest one. It foresees the opportunity to connect systems using APIs and share health data in live time. HL7 messages are composed by following defined rules. Medical documents shared between different systems have a specific structure and can be created using templates.
Hire HL7 software development experts

Business First
Code Next
Let’s talk
FAQ
HL7 is a set of standards that help share and retrieve health data. Messages composed of defined rules can be exchanged by digital systems that use different technologies.
Usually, HL7 messages are used to connect many diverse digital solutions from different vendors into one system. Also, the use of HL7 standards enables medical institutions to share information with other hospitals, insurance companies, or regulatory agencies.
Three primary versions of HL7 messaging standards are the following:
- HL7 V2 — the most widespread version
- HL7 V3 — an enhanced version of the HL7 V2
- HL7 CDA — medical documents creation markup
- HL7 FHIR — the newest version
There are many benefits of adopting the HL7 standard to enable health data interoperability. The foremost advantages are the following:
- Smooth data integration across different systems
- Better clinical data quality
- Reduced errors
- Improved HL7 compliance
- Automated health information exchange
- Improved collaboration
The HL7 EHR functional model is a framework for message creation and medical document creation. In a nutshell, it is a set of rules that help create unified messages exchanged between systems that use different technologies.
Build your ideal
software today